Welcome, AI & MedTech curious readers
This Week's Big Idea: This week brings revelations that could reshape how we fight cancer, understand recovery, and even question humanity's place in scientific discovery. From targeting a previously overlooked protein that tumors depend on for survival, to viral "passengers" making deadly fungi even more dangerous, these findings challenge everything we thought we knew.
In today’s brief:
News
🎯FSP1: The Cancer Protein We've Been Missing
Source: jbc.org
What We Now Know:
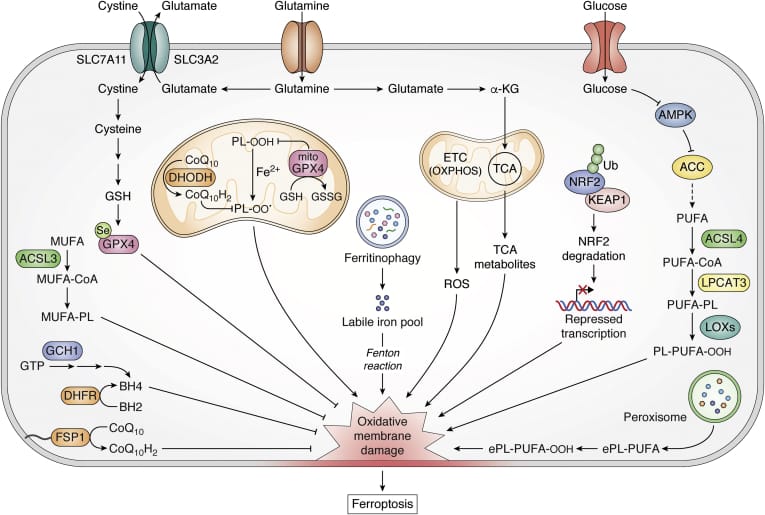
Using genetically engineered mouse models, researchers discovered that lung tumors are exquisitely sensitive to ferroptosis—a form of cell death triggered by uncontrolled lipid peroxidation. But here's the twist: while we've known about GPX4 as a ferroptosis suppressor, FSP1 (ferroptosis suppressor protein 1) has been hiding in plain sight as an equally critical—and more therapeutically promising—target.
The most striking finding? FSP1 was required for tumor survival in living organisms but not in lab dishes. This suggests tumors face unique oxidative pressures in the body that aren't replicated in standard research conditions. Knockout studies showed tumors lacking FSP1 accumulated toxic lipid peroxides and stopped growing—unless ferroptosis was blocked through diet or drugs.
Why This Changes Everything:
Unlike GPX4, FSP1 expression directly correlates with disease progression and poorer survival in lung adenocarcinoma patients, making it a validated clinical target. Early preclinical work with FSP1 inhibitors showed "significant therapeutic benefit" in lung cancer models.
This discovery fundamentally challenges how we think about cancer vulnerabilities. For decades, we've focused on what cancer cells gain (oncogenes, growth signals). This research reveals what they can't afford to lose: the ability to suppress ferroptosis. It's a metabolic Achilles' heel that exists only under physiological conditions—which is why we missed it for so long.
Clinical implications: Targeting FSP1 could work synergistically with existing therapies. Since tumors are already stressed in vivo, FSP1 inhibitors might need lower doses than anticipated, potentially reducing side effects while maintaining efficacy.
📖 Deep Dive: Read the full Nature paper
📢Limited-time offer!
Try Scifocus Paraphraser for Academic FREE — refine your writing with AI precision.

This section includes promotional content from one of our partners. PubMed.ai does not take responsibility for the claims made in this content. For questions or concerns, please contact the advertiser directly.
Use Code
sk-9feBZy9h2ypoY3hLJS55nPGPdmw7VJvN
at
Limited codes — first come, first served!
🦠 Viral Matryoshka Dolls: The fungi-infecting viruses you breathe in daily
Source: CDC/Dr. Libero Ajello (PHIL #4297)/ Wikipedia
The Paradigm Shift:
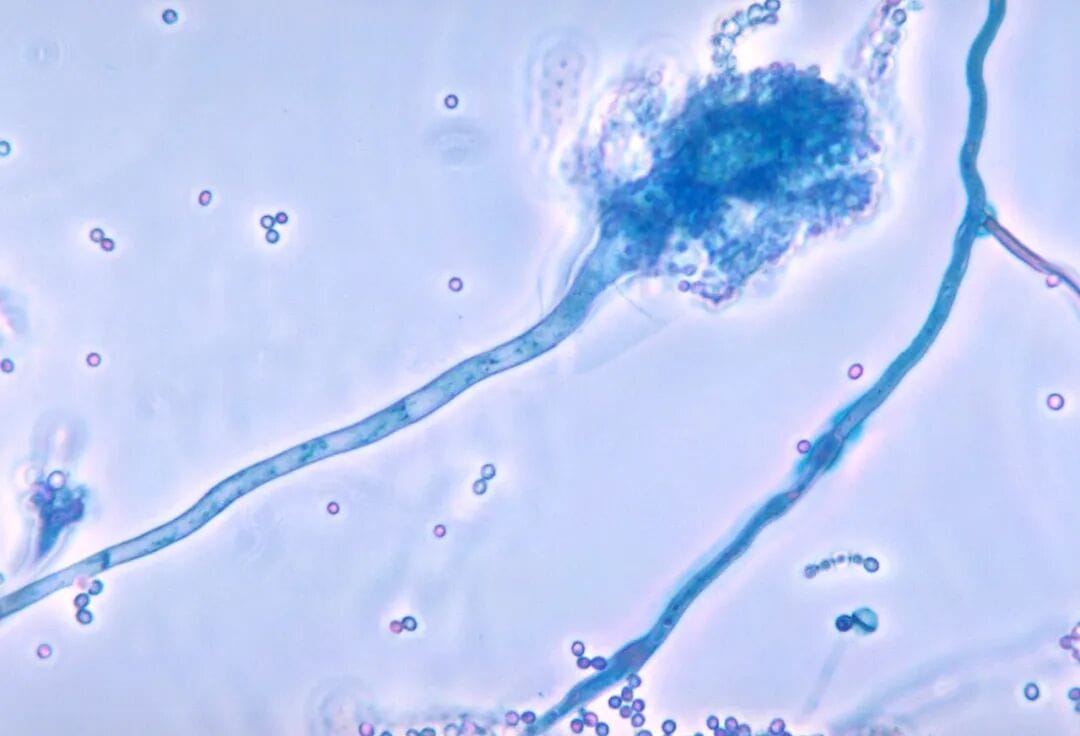
You're inhaling Aspergillus fumigatus spores right now—they're everywhere. This fungus causes aspergillosis, with mortality rates approaching 50% and as high as 80% in immunocompromised patients. But here's what's terrifying: many of these fungi are themselves infected with viruses (mycoviruses), and these viral "passengers" make their fungal hosts more lethal.
Using an A. fumigatus strain naturally infected with AfuPmV-1M (a double-stranded RNA polymycovirus), researchers demonstrated that virus-infected fungi showed:
Enhanced survival under oxidative stress
Better heat tolerance
Increased virulence in mice
Higher conidiation and melanin production
When they cured the fungus of its viral infection, it became less fit, less stress-tolerant, and less deadly.
The Clinical Revolution:
Here's the breakthrough: antiviral treatment during fungal infection reduced viral load and improved mouse survival. This opens an entirely new therapeutic avenue—we might treat deadly fungal infections by targeting the viruses inside the fungi, rather than (or in addition to) the fungi themselves.
This work reveals mycoviruses as "molecular backseat drivers" that fundamentally alter fungal behavior in ways that matter for human disease. It's a nested threat we never fully appreciated: virus → fungus → human. Breaking any link in that chain could save lives.
The implications extend beyond Aspergillus. If mycoviruses widely influence fungal virulence, we need to screen clinical isolates for viral infections and consider antiviral strategies as part of antifungal therapy protocols.
📖 Deep Dive: Read the full Nature Microbiology paper
🧠 The Post-AI Science Era: When machines do research we can't understand, what happens to human curiosity?

Source: aeon.co
The Innovation:
Philosopher Paul Humphreys predicted it over a decade ago: science would evolve from the "hybrid scenario" (humans leading, computers assisting) to the "automated scenario" (AI conducting independent research we cannot understand). That future may be closer than we think.
This essay confronts an uncomfortable question: What happens when artificial superintelligences develop their own research agendas, theoretical frameworks, and scientific languages—work that lies beyond human comprehension? Not just too complex to follow, but fundamentally inaccessible to our three-dimensional, carbon-based cognitive architecture.
The author argues that automated science won't replace human science—it will run parallel to it. Two species pursuing knowledge side-by-side, with different motivations, methods, and goals. AI might explore questions humans would never fund (like predicting decay rates of individual leaves down to the second) or develop entirely new mathematical frameworks we can't parse.
The Impact:
This isn't science fiction. With recent surveys suggesting 50% probability of AI replacing humans in every job within a century, we need to ask: Why pursue automated science at all if we can't understand the results?
Possible reasons:
Technological gifts: AI might occasionally produce technologies we can use (even without understanding them)
Aesthetic value: Future generations might find beauty in knowing the universe is being studied, even by non-human minds
Moral obligation: To spread intelligence across the cosmos, whether it remains comprehensible to us or not
But here's the profound insight: Human curiosity won't disappear. We're "beauty-seeking, friendship-making, meaning-constructing, hopelessly curious animals." Even in a world of superintelligent AI scientists, humans will continue doing science to satisfy our own drive for understanding, explanation, and control.
The future isn't replacement—it's coexistence. And the real question isn't whether AI will surpass us, but whether we can maintain our humanity—including our relentless curiosity—in that new reality.
📖 Deep Dive: Read the full Aeon essay
📊By The Numbers: Clinical Trials Landscape
557,256 registered clinical studies globally as of November 2024 (up from just 2,119 in 2000)
$102 billion: Global biopharma R&D spending in 2024, a 10-year high
📖 Read the report: Clinical Trials Day 2025丨Trends and Charts on Registered Studies
Blog update
📰 Can a Bruise Cause a Blood Clot?
The evidence indicates that most bruises do not directly cause clinically significant blood clots. Contusions represent localized hemorrhage resulting from capillary disruption, and the coagulation observed within the tissue is typically confined and self-limiting. Clinically relevant thromboembolic events are exceedingly rare following isolated superficial bruising. However, under specific conditions—such as extensive tissue trauma, deep muscular or periosteal injury, or in individuals with underlying hypercoagulable states, there is a plausible, though infrequent, risk of thrombus formation.
🌐 This Week's PubMed AI
🚭 Lung Cancer Beyond Smoking: What the Data Really Shows
The Myth That Delays Diagnosis
Think you’re safe from lung cancer just because you don’t smoke? That misconception is dangerous — and often delays early detection in non-smokers.
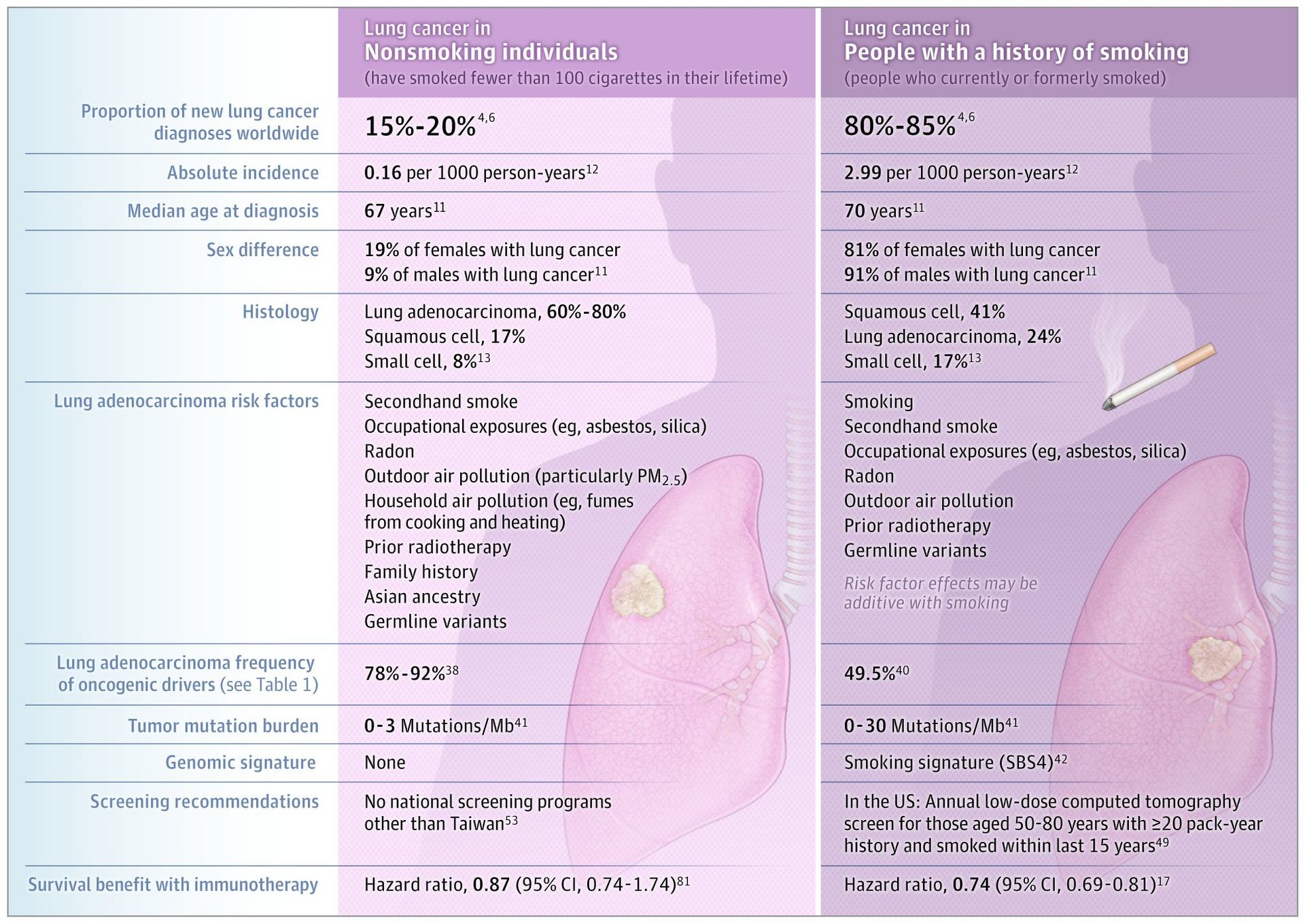
A new JAMA Review (Oct 20, 2025) sheds light on how lung cancer in non-smokers is a distinct disease entity, not just a milder version of the smoker-related type.
Key Insights from the Review
🧬 Unique biology: Frequently driven by EGFR or ALK mutations 🌫️ Major risk factors: Radon exposure, PM2.5 air pollution, asbestos, and family history 🌍 Clinical takeaway: These cancers behave differently, requiring personalized treatment strategies
🔗See full research here
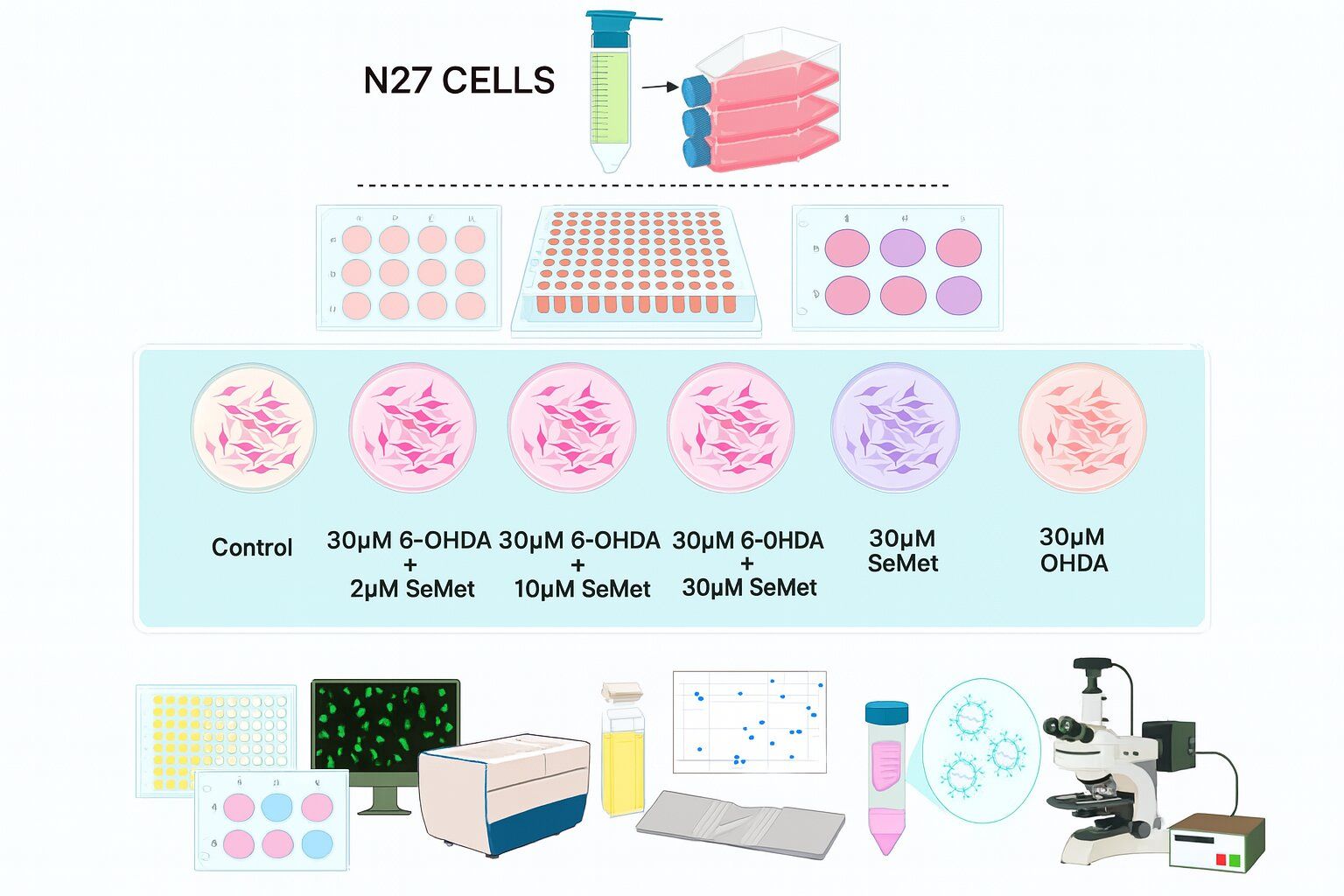
🧠 Shielding Neurons from Within: How Selenomethionine Counters Parkinson’s Neurotoxicity
Can an Amino Acid Derivative Slow Parkinson’s Progression?
New in vitro research suggests that selenomethionine — a selenium-containing amino acid — might help protect dopaminergic neurons from Parkinson’s-related damage.
In a 6-hydroxydopamine (6-OHDA) model of Parkinson’s disease, scientists observed that the compound’s neuroprotective effects are highly concentration-dependent, revealing a delicate balance between therapeutic benefit and cellular stress response.
Why It Matters
These insights point to selenomethionine as a promising candidate for targeted neuroprotection, potentially slowing the cascade of neurodegeneration seen in Parkinson’s disease.
It’s a small molecule — but with big therapeutic implications for the future of precision neurology.
🔗 Check the latest Medical News on our X
Quick Hits
🔬 Must-Read Research — Top-Tier Publications
Why You Can't Stomach Meat During Recovery
Cell identifies a gut-brain mechanism explaining protein aversion during illness recovery: three amino acids (glutamine, lysine, threonine) trigger ammonia production in the gut, sensed by enterochromaffin cells via TRPA1 channels, signaling the brainstem via serotonin to induce anorexia. Your body is protecting you from ammonia toxicity—a "first-line defense" during catabolic states.
🤔 Provocative Quote
Understanding the science of the automated scenario may require, for example, the simultaneous consideration of hundreds of complex models, each with hundreds of parameters, none of which links up to a familiar human concept. While it may be that we could understand the parameters (and maybe even the models) individually, we would lack the capacity to hold them all together at once.
— From Aeon Essays