Welcome, AI & MedTech curious readers
This Week's Big Idea: A groundbreaking Stanford study published in Nature Aging shatters conventional wisdom about cancer and age. While cancer risk rises through our 60s and 70s, it mysteriously drops in centenarians. The reason? Aging itself becomes tumor-suppressive. In mouse models, aged tissue actively repressed oncogenic KRAS-driven lung tumors and weakened the impact of many tumor suppressor gene losses—especially PTEN. The finding reveals that extreme aging fundamentally rewires cellular biology in ways that protect against cancer, offering a biological explanation for the "oldest-old paradox."
In today’s brief:
News
🧬 Nature: Why Centenarians Rarely Get Cancer—Aging Actively Suppresses Tumors
Source: nature.com
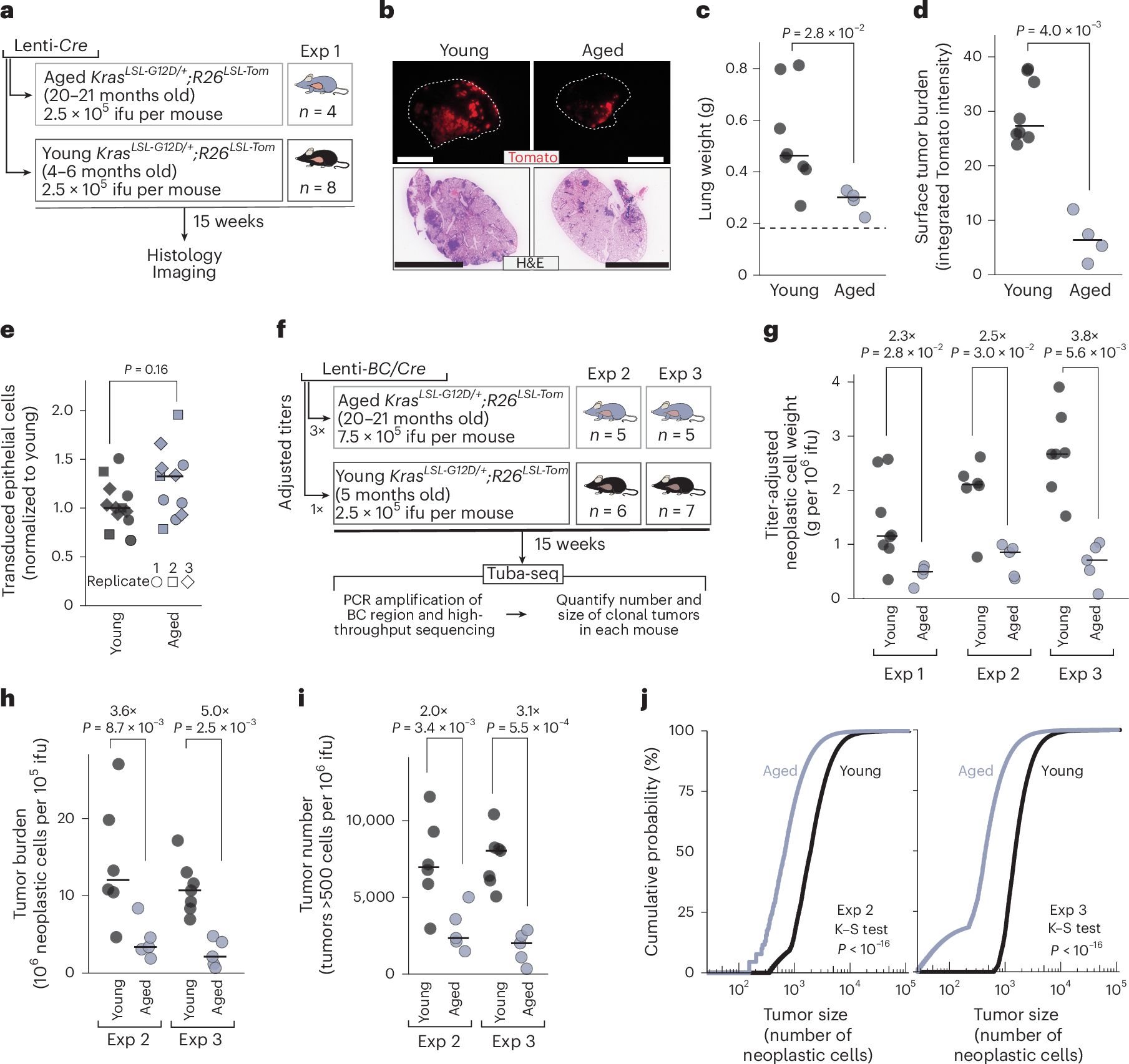
What We Now Know: Aging doesn't just correlate with cancer—it has a biphasic relationship. While mutation accumulation drives cancer risk upward through middle age, extreme aging (90+) creates a profoundly tumor-hostile environment. Stanford researchers using genetically engineered mouse models found that aged tissues actively suppress oncogenic KRAS-driven lung tumor initiation and growth. More strikingly, aging diminished the cancer-promoting effects of inactivating key tumor suppressors, with PTEN loss showing disproportionately weakened impact in aged mice.
Why This Changes Everything: Single-cell transcriptomic analysis revealed that neoplastic cells in aged mice retain age-related transcriptomic signatures even after oncogenic transformation—meaning the "age state" persists through cancer development. When PTEN was inactivated, it paradoxically reversed aging signatures in both cancer cells and the tumor microenvironment. This suggests aging and cancer pathways are deeply interconnected, and that the extreme longevity phenotype may protect against tumorigenesis through mechanisms beyond simple immune surveillance decline.
✍️Try Scifocus AI Humanizer for FREE!
Elevate your writing with clarity, tone, and human-level polish.

This section includes promotional content from one of our partners. PubMed.ai does not take responsibility for the claims made in this content. For questions or concerns, please contact the advertiser directly.
Use Code
sk-7YkUV1ThrAWqIq73OoyhVaoG5Czd4GZH
Limited codes — first come, first served!
🧠Biohacking: Why Restricting Oxygen Actually Spikes Executive Function
Source: onlinelibrary.wiley.com
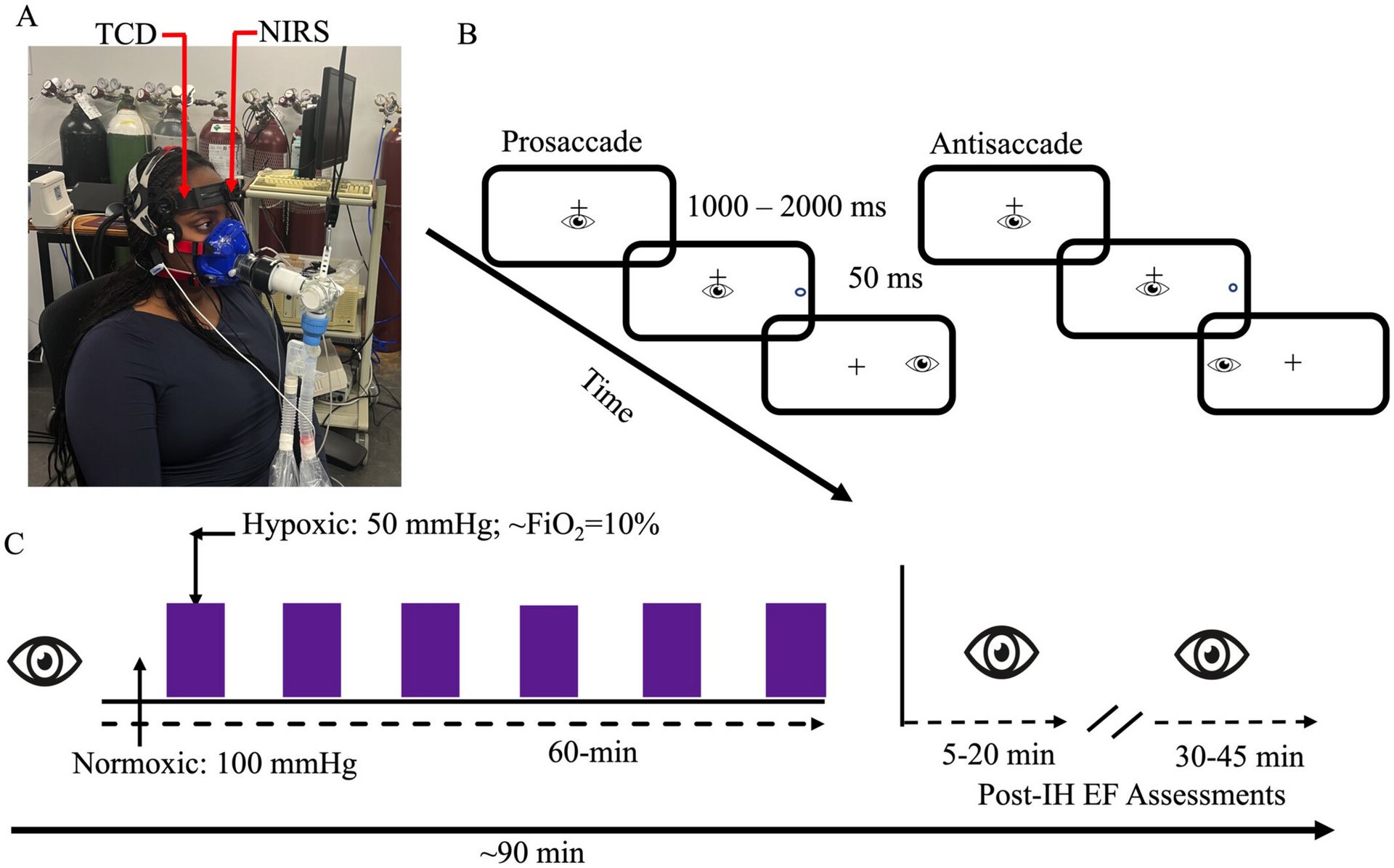
The Innovation: A single 60-minute intermittent hypoxia session (alternating 5-minute cycles of normal and reduced oxygen) produces a surprising delayed effect: executive function improves significantly 30-45 minutes after the protocol ends. University of Western Ontario researchers found a 6% reduction in reaction times on demanding cognitive tasks, with increased cerebral blood flow during the hypoxic intervals. Critically, the benefit appears selectively in high-level executive function, not basic processing.
The Real-World Impact: This is the first evidence that a single hypoxia session can boost brain performance—previous studies required weeks of training. The mystery deepens: the cognitive benefit didn't correlate with any single physiological change measured during hypoxia. Researchers suspect the effect involves complex interactions between blood flow, biomolecules like nitric oxide, and enhanced neural network connectivity. This opens pathways for accessible cognitive enhancement, especially for populations with mobility limitations who can't exercise traditionally.
⚖️ AI Medical Liability Crisis: Doctor, Hospital, or Programmer. Who Gets Sued?

Source: theguardian.com
The Paradigm Shift: As AI systems proliferate in clinical diagnosis, a massive legal vacuum has emerged. The 2024 JAMA AI Summit report reveals the complexity: When an AI-assisted diagnosis goes wrong, is it the physician who relied on the system? The hospital that deployed it? The software company? Or the data scientists who trained the model? Harvard Law's Prof. Glenn Cohen warns patients face severe barriers proving fault due to AI's "black box" nature and challenges in accessing information about the system's inner workings.
The Clinical Revolution: Traditional malpractice law assumes clear human decision chains. AI shatters this. Stanford Law's Prof. Michelle Mello notes courts can resolve these issues, but early inconsistencies will elevate costs across the innovation ecosystem. A critical gap: many AI tools escape FDA oversight, and the "best-evaluated tools have been least adopted while most-adopted tools have been least evaluated." The legal framework being debated—medical device liability versus decision-support tool responsibility—will fundamentally reshape healthcare innovation's future.
FYI
🌍 By The Numbers: Antibiotic Resistance Reaches Crisis Levels
1 in 6: The number of laboratory-confirmed bacterial infections worldwide that were resistant to antibiotic treatments in 2023.
5–15%: The average annual increase in antibiotic resistance across monitored pathogen combinations.
The Warning: The WHO's new October 2025 report warns that resistance to essential antibiotics (including last-resort treatments like carbapenems) is outpacing modern medicine, particularly in the South-East Asian and Eastern Mediterranean regions.
Blog update
📰 How Long Do Manic Episodes Last?

Based on the Diagnostic and Statistical Manual of Mental Disorders (DSM-5-TR) criteria, a full manic episode must last at least seven days (or any duration, if severe enough to necessitate hospitalization). However, if left untreated, the natural course of a manic episode can stretch to three to six months; with active, standard pharmacological treatment, acute symptoms are typically brought under control within four to eight weeks.
🌐 This Week's PubMed AI
🧬 The Hidden Survival Engine of Lung Cancer: Why FSP1 Changes Everything
A Breakthrough From Two Nature Papers
For years, GPX4 has dominated the conversation around ferroptosis in lung cancer.
But new evidence now shows we may have been looking at the wrong target.
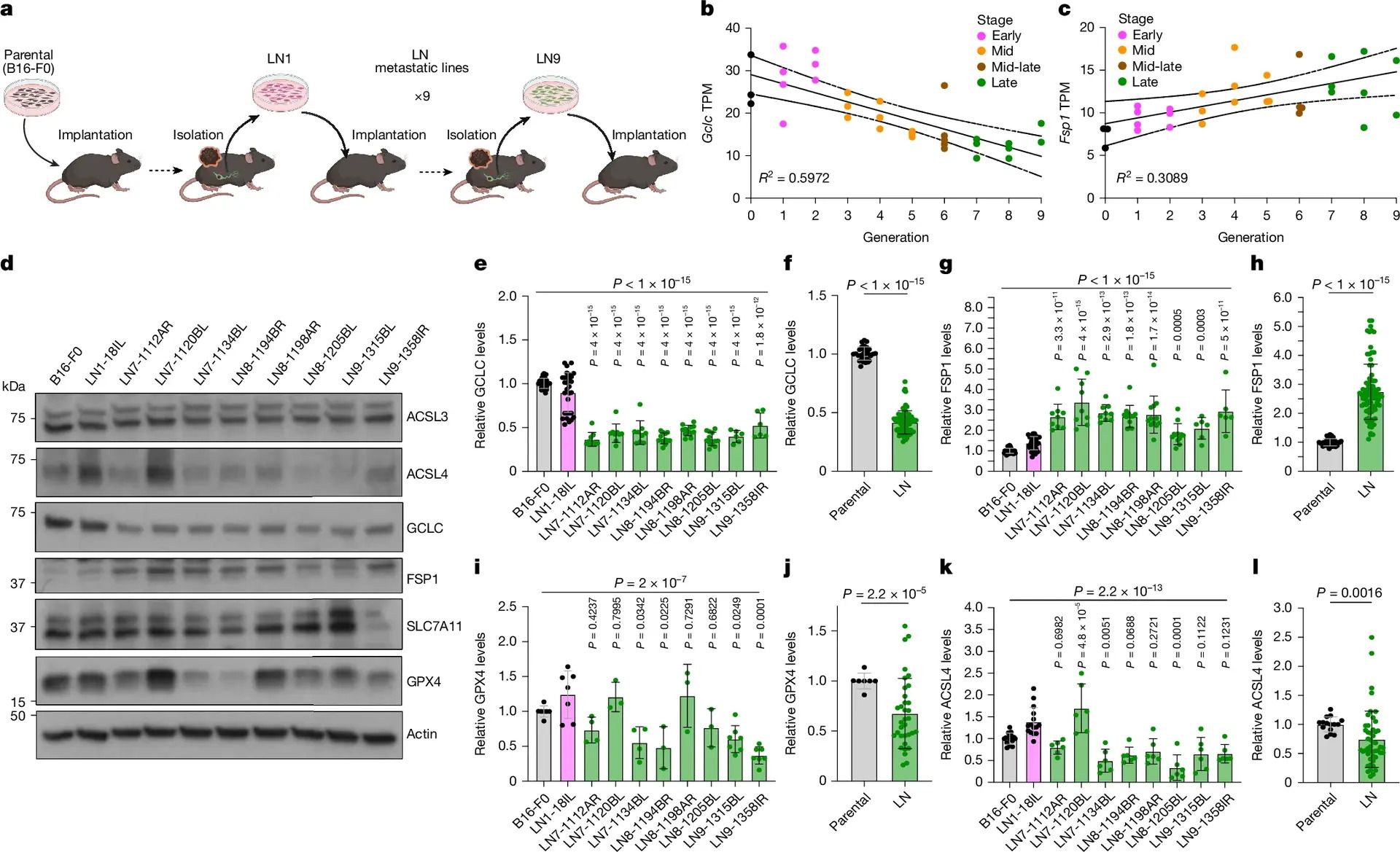
A Nature double-paper reveals that lung tumors rely heavily on FSP1—not GPX4—to suppress ferroptosis in vivo.
Why This Discovery Matters
Biology inside the human body behaves differently than in a dish. These studies show:
🧫 Target GPX4 in vitro → tumors die
🧍 Target GPX4 in vivo → tumors survive… unless FSP1 is blocked
FSP1 is the missing link — the true in-body survival mechanism. This shifts how we understand ferroptosis vulnerability and future therapeutic strategies.
Check the latest Medical News on our X
🧐The Bigger Message: Context Matters
When a single difference between in vitro and in vivo biology can overturn an entire treatment paradigm, one thing becomes clear:
Static, general-purpose AI isn’t enough for medical science. Research evolves every day, and shallow knowledge quickly becomes outdated.
How PubMed.ai Helps
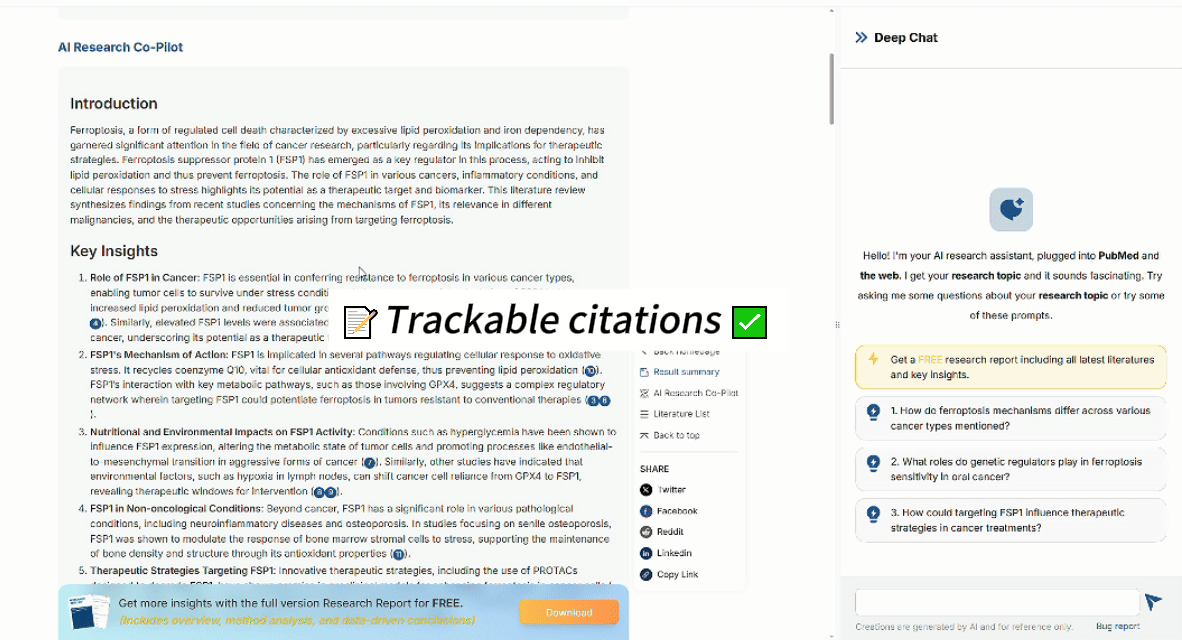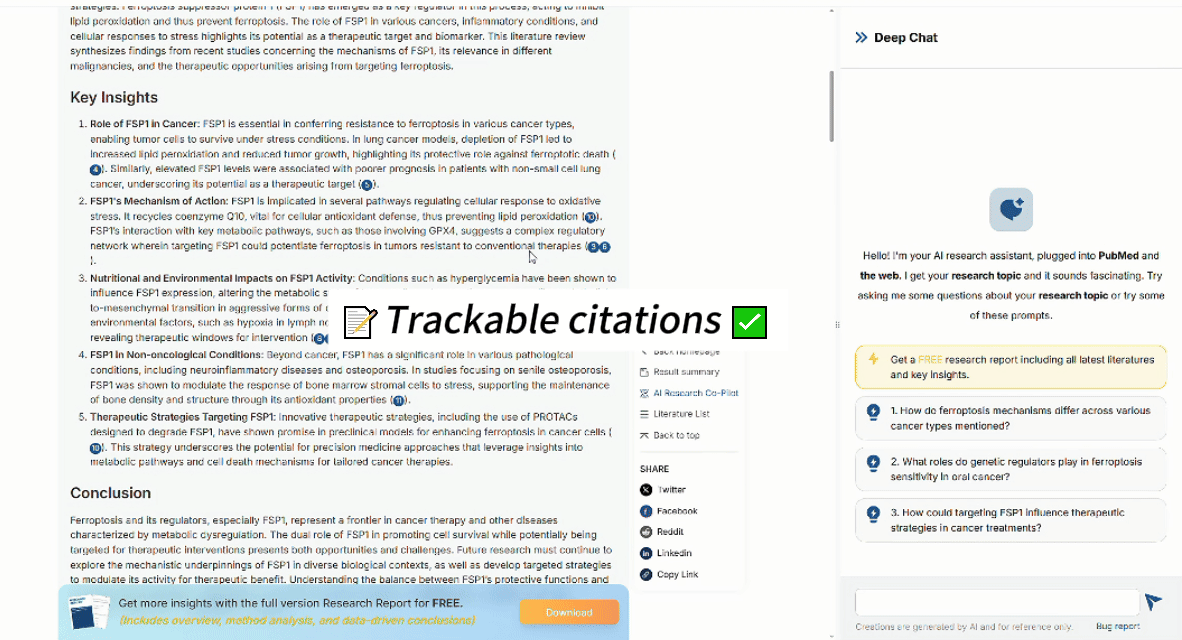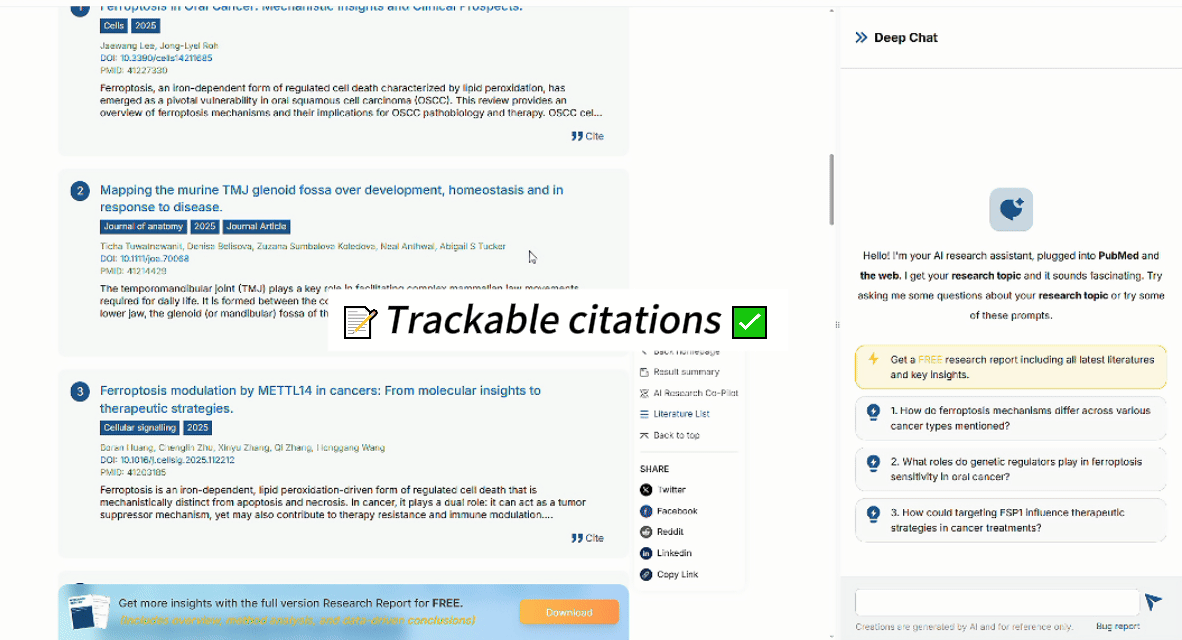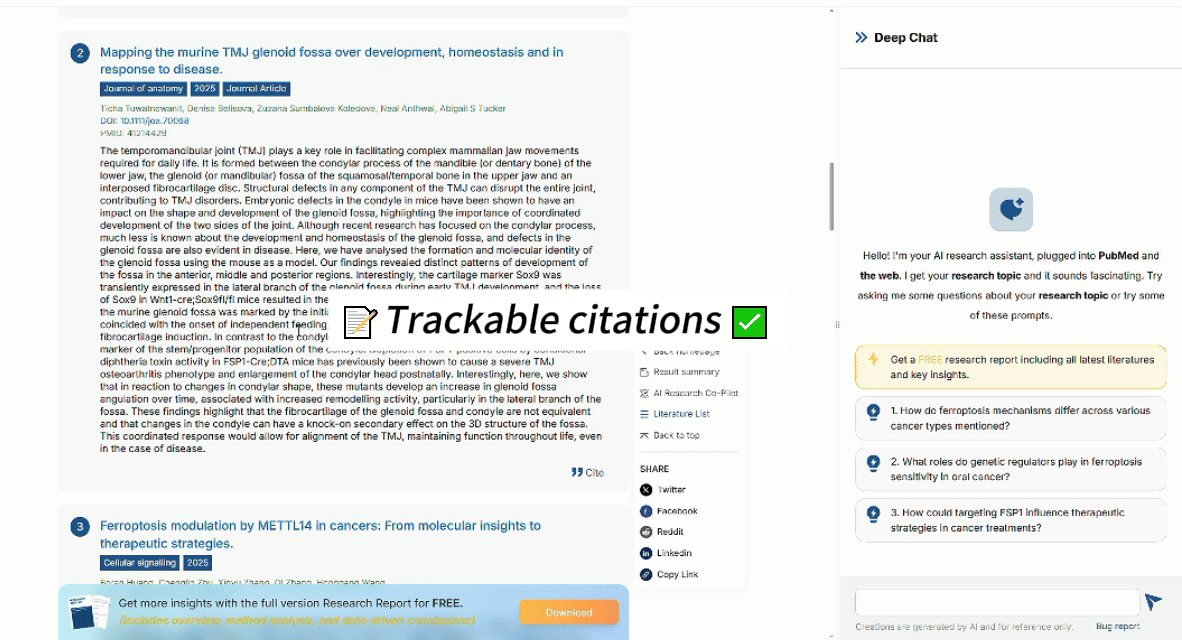
PubMed.ai indexes the latest biomedical papers in real time, interprets biological context, and gives you precise, citable answers instantly.
Try searching: “FSP1 ferroptosis lung cancer” You’ll immediately see why context-aware search matters.
See full research here
Quick Hits
🔬 Must-Read Research — Top-Tier Publications
🤔Provocative Quote
We thought aging was just accumulating damage. Turns out, the body's oldest cells are also its wisest, they know how to say no to cancer
— Editorial tagline