Welcome, AI & MedTech curious readers
This Week's Big Idea: What if the biggest threat to your mental health wasn't a chemical imbalance, but a secret betrayal happening at the cellular level? We're peeling back the layers on the brain's hidden puppet masters, the cells that can be programmed to turn against you. Let's get into it.
In today’s brief:
News
🧠 The Brain's Secret Betrayal: Scientists Prove Astrocytes Turn Stress Into Mental Illness
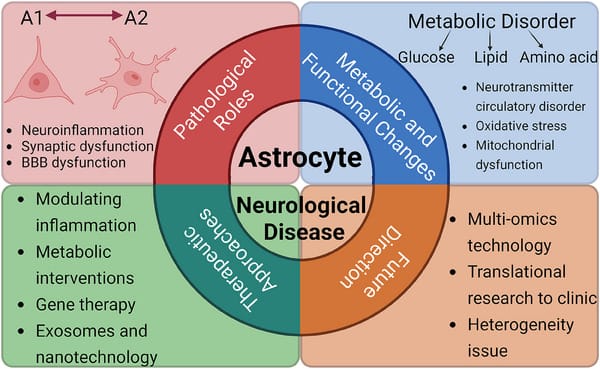
Source: pmc.ncbi.nlm.nih.gov
The Core Finding: In a groundbreaking 2025 study, researchers discovered that astrocytes—star-shaped support cells comprising 40% of your brain—don't just support neurons. They actively hijack stress responses, transforming normal life pressures into psychiatric disorders. Using advanced cellular imaging, scientists showed these "helper" cells become mental health saboteurs.
Why This Changes Everything:
A Revolution in Psychiatry: This opens the door to treating mental illness by targeting astrocytes instead of neurons, potentially reversing decades of psychiatric damage.
Stress as Cellular Programming: Early life trauma literally reprograms these cells into "psychiatric time bombs" that activate years later during minor stress.
Redefining Mental Resilience: This research fundamentally explains why identical stressors break some people while others thrive—it's all about your astrocyte programming.
Smarter Writing, Faster Research, Better Results

This section includes promotional content from one of our partners. PubMed.ai does not take responsibility for the claims made in this content. For questions or concerns, please contact the advertiser directly.
🎮 Reshaping Motor Memory: Neural Circuits Shift from Random to Efficient During Learning
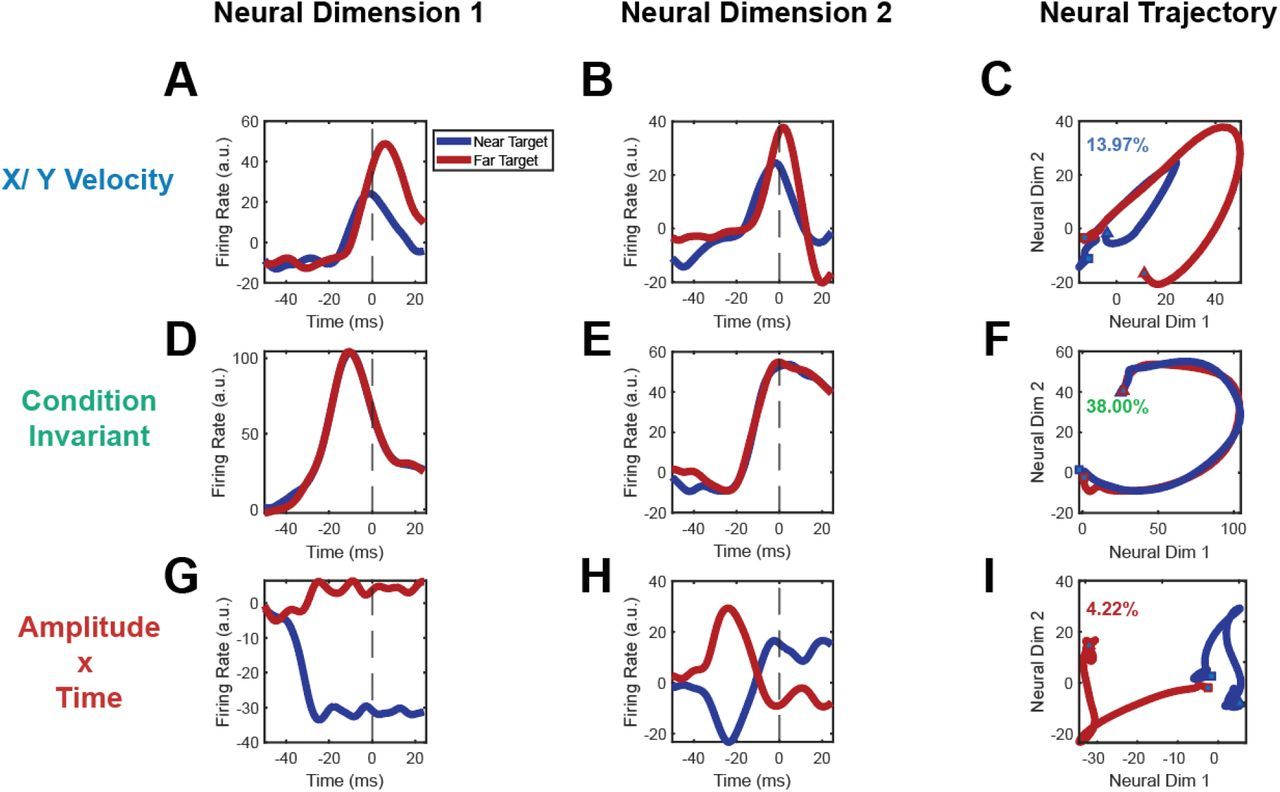
Source: biorxiv.org
The Pivotal Study: In a 2025 experiment, researchers recorded neuronal ensemble activity in the primary motor cortex of rodents learning a skilled reaching task and validated key findings in human volunteers with non-invasive EEG. Early learning phases exhibited high-dimensional, exploratory neural patterns that gradually collapsed into low-dimensional, stereotyped trajectories optimized for precise movement. These neural refinements correlated with a 40% reduction in task completion time and a 30% decrease in movement variability.
Key Implications: Insights into optimizing rehabilitation protocols, improving brain–machine interface training, and understanding motor disorders.
Deep Dive: Neural trajectories improve motor precision
🤖 AI-Driven Science: AI-Powered Exoskeleton Enhances Movement Prediction
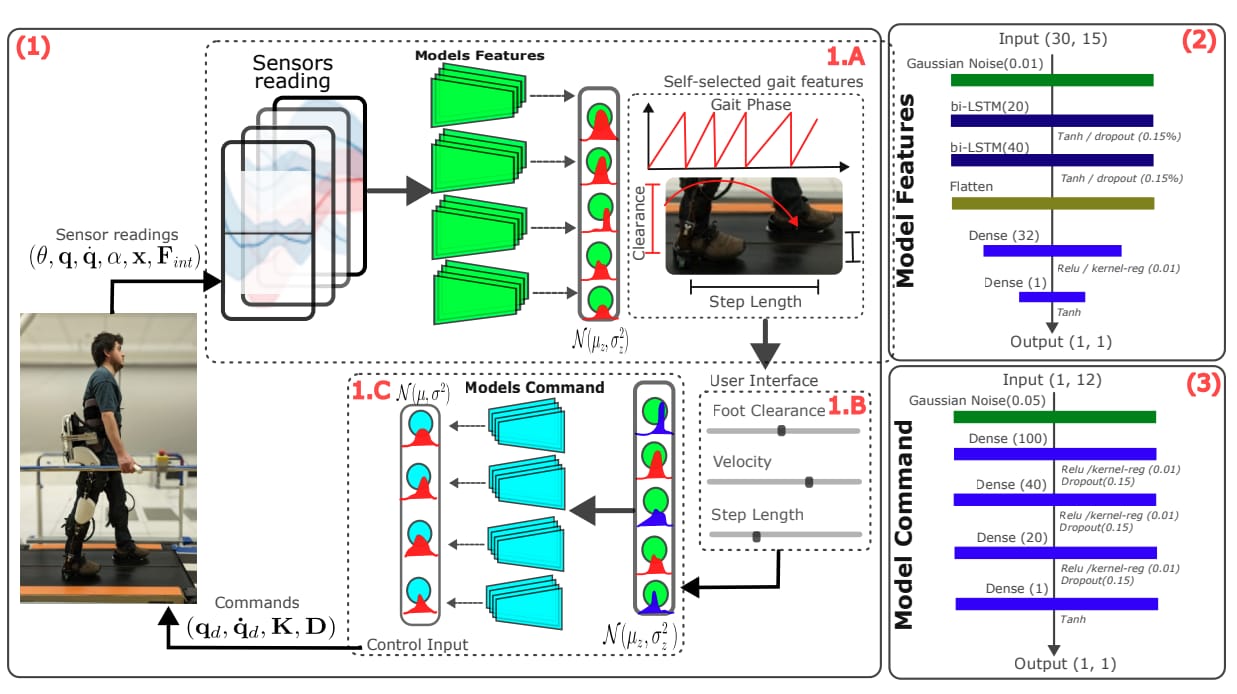
Source: arxiv.org
The Innovation: A recent study integrated a deep neural network into a lower-limb exoskeleton that leverages real-time electromyography (EMG) and inertial measurement unit (IMU) data to predict user gait intentions with 95% accuracy and adjust assistance dynamically. Clinical trials with post-stroke patients demonstrated a 20% improvement in walking speed and a 15% reduction in metabolic cost compared to passive exoskeletons.
Key Implications: Personalized rehabilitation for varied terrains, enhanced mobility in neurological patients, and scalable tele-rehabilitation solutions.
FYI
🌍 By The Numbers:
US$ 12.40 billion: The projected value of the global brain-computer interface (BCI) market by 2034, as the technology moves from science fiction to clinical reality for restoring function.
5.4 million: The number of people living with paralysis in the U.S. alone, representing a major population that could regain movement and communication abilities through advanced BCI systems.
📖 Complete Analysis: Brain Computer Interface Market Size and Forecast 2025 to 2034 & Paralysis in the U.S.
Blog update
S/P Medical Abbreviation: Everything You Need to Know

Medical charts are often dense with abbreviations that can confuse even seasoned clinicians. One of the most frequently encountered—and potentially misunderstood—notations is S/P, shorthand for “status post.” This article explores the meaning of S/P, its applications across specialties, and the distinction between S/P and Standardized Patients (SPs) in medical education.
This Week's PubMed AI
Top Research for you
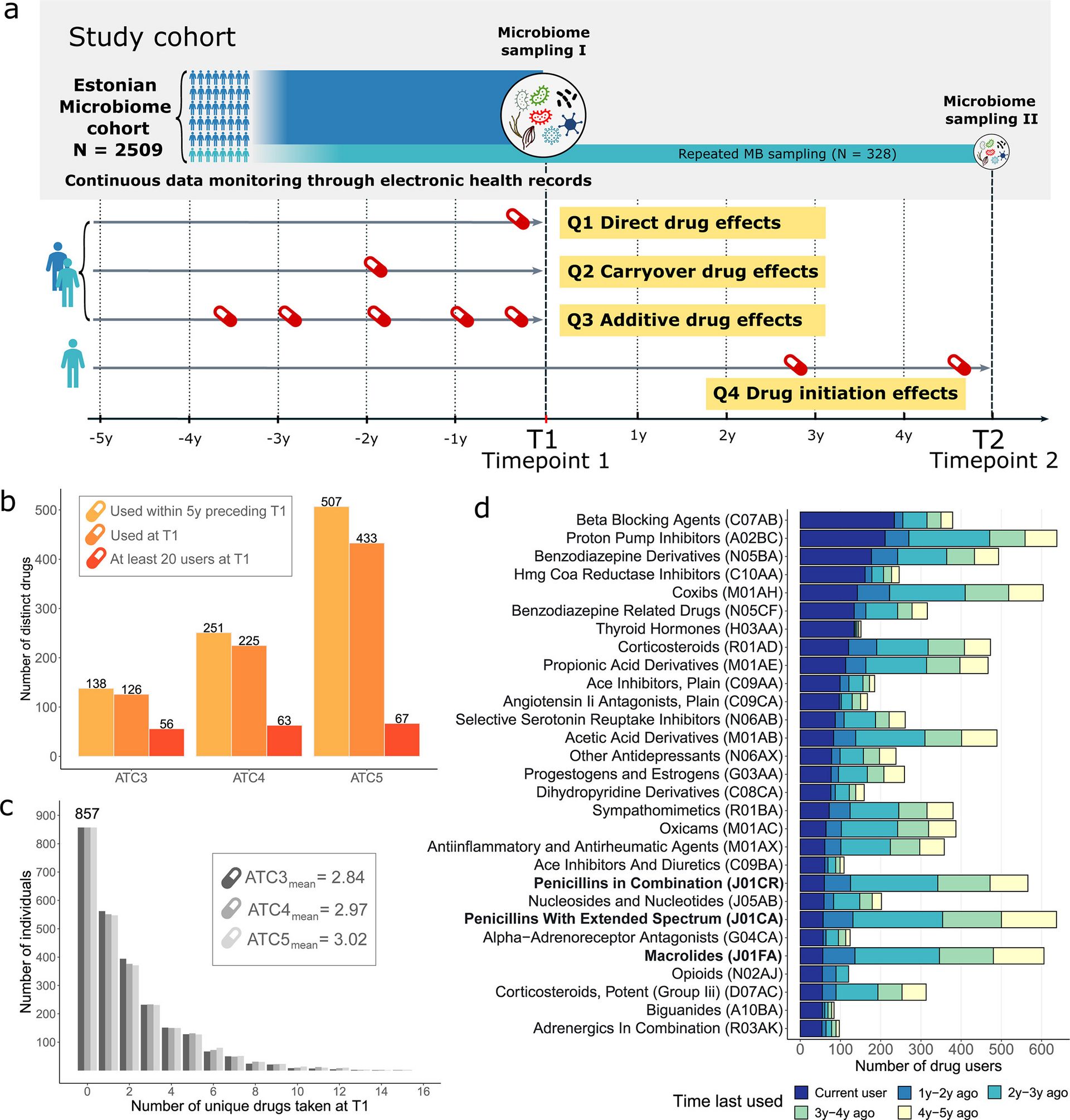
Medications Leave a Lasting Mark on the Gut Microbiome — Long After Use
Key Mechanistic Findings:
Persistent Dysbiosis: Alterations in microbial community structure remain detectable long after treatment ends.
Functional Disruption: Shifts in metabolic pathways, including short-chain fatty acid production and bile acid metabolism.
Host Interactions: Links between microbiome perturbations and chronic inflammatory or metabolic conditions.
Broader Impact:
Calls for integrating microbiome assessments into drug safety profiles.
Highlights the microbiome as both a therapeutic target and a biomarker for long-term health outcomes.
Raises the need for mitigation strategies to restore microbial balance post-medication.
Follow our X to get the latest Medical Information!
September 17 is World Patient Safety Day
Safety first, always.
Healthcare systems must protect patients, reduce harm, and build trust.

⚠️ Did you know?
➡️ 1 in 10 patients is harmed while receiving hospital care.
Patient safety is not simply about avoiding errors—it is about building resilient systems. This includes training healthcare professionals in safety culture, adopting digital health tools to improve monitoring, encouraging open communication about mistakes, and, crucially, involving patients themselves as active partners in their care. When patients are empowered to voice concerns and participate in decision-making, care becomes more transparent, accountable, and effective.
The theme of World Patient Safety Day 2025 emphasizes collaboration: clinicians, policymakers, and patients must work together to create environments where safety is not a checklist, but a core value that guides every action. As healthcare grows more complex, maintaining trust depends on our ability to minimize harm and place safety at the heart of innovation.
Join our Facebook Group to communicate with more talented researchers!
Quick Hits
Must-Read Research — Top-Tier Publications
Provocative Quote
Biology is no longer destiny; it is a dialogue
— Editorial tagline